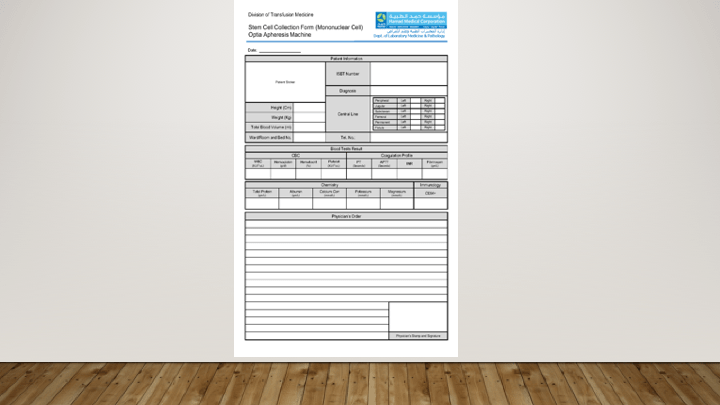
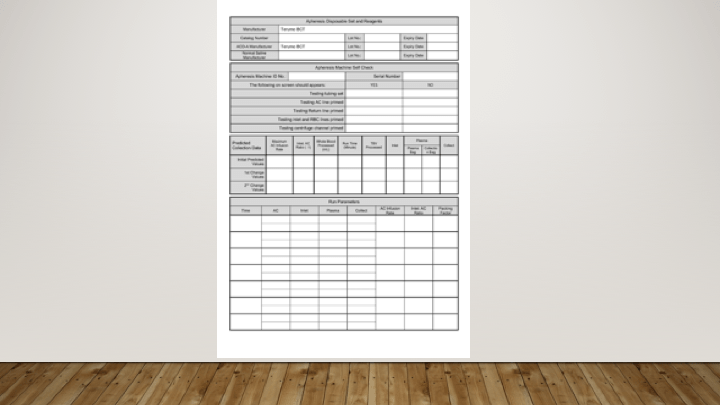
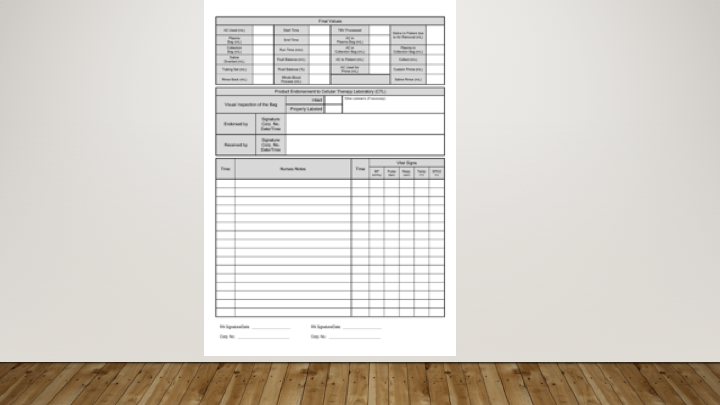
The donor module of Medinfo includes recruitment, logistics, registration, donor screening, collection, marker testing, donor immunohematology, and component production. There is also a module for inter-depot transfer of blood units from the donor center to the hospital end-users.
The patient module includes patient testing (ABO/D typing, antibody screen, antibody identification), direct antiglobulin test, elution, component modification (washing, aliquoting, pooling), allocation/reservation of blood components for a patient, release of blood components, and their return.
Some sites elect to use their laboratory system’s blood bank module in conjunction with Medinfo donor module. In this case, they receive each and every unit into their laboratory blood bank module and do all patient activities in it. There is no link between patient and donor module. They will have to monitor and transfer inventories in their laboratory system.
At a site using integrating both the donor and patient modules of Medinfo, they will be able to track units across the system to any hospital blood bank. They will have access to the rules-based system to generate algorithms for use of blood components based on user-defined criteria. They can instantly perform look back of donor units associated with adverse effects, and be able to rapidly quarantine components subject to recall from the manufacturer or product incidents. Here are some examples of this functionality:
Example 1: The hematologists want all their patients to receive leukodepleted irradiated RBCs and platelets at a site not using pathogen-inactivation. Medinfo can prepare an algorithm by site, clinical diagnosis, or other criteria which will block release of those components that are not irradiated and leukodepleted. Blood Bank staff will not be able to release anything else. The donor module can prepare customized component or modification can take place in the hospital blood bank.
Example 2: During production, it is discovered that units prepared in one of the centrifuges (or automated component equipment Reveos) became contaminated with a foreign substance. In Medinfo. In Medinfo, all units prepared during the affected time interval can be immediately quarantined across the system including all hospital blood banks and thus prevent their being transfused.
Example 3: A patient has developed hepatitis C after transfusion. Using the transfusion history, one can retrieve data on all transfused units. The entire production process can be reviewed for each unit, including donor marker testing. If a unit is implicated, then all patients receiving other components from that donor can be immediately identified for follow-up.
If a disaster occurs, one can quickly check Medinfo’s cumulative stock display of all components at all sites—donor unit and all hospital blood banks. One can initiate transfer of units from unaffected sites to the disaster location. This can be updated as frequently as needed—within seconds!
There are probably ways to accomplish this by using the laboratory information system, but it will be slower and require separate communication to the Medinfo donor site. There will be no seamless integration and delay.
In summary, there are many advantages to using both donor and patient Medinfo modules. Even at sites where there was separate transfusion service functionality, I elected to use both modules together for seamless integration. It would be very time-consuming to manually check between the laboratory and Medinfo donor module. Medinfo’s patient module offers has strong safeguards to prevent release of untested or partially tested units (example: release of Kell-untested RBCs to a patient with anti-Kell) and a very robust electronic (computer) crossmatch.
11/10/20