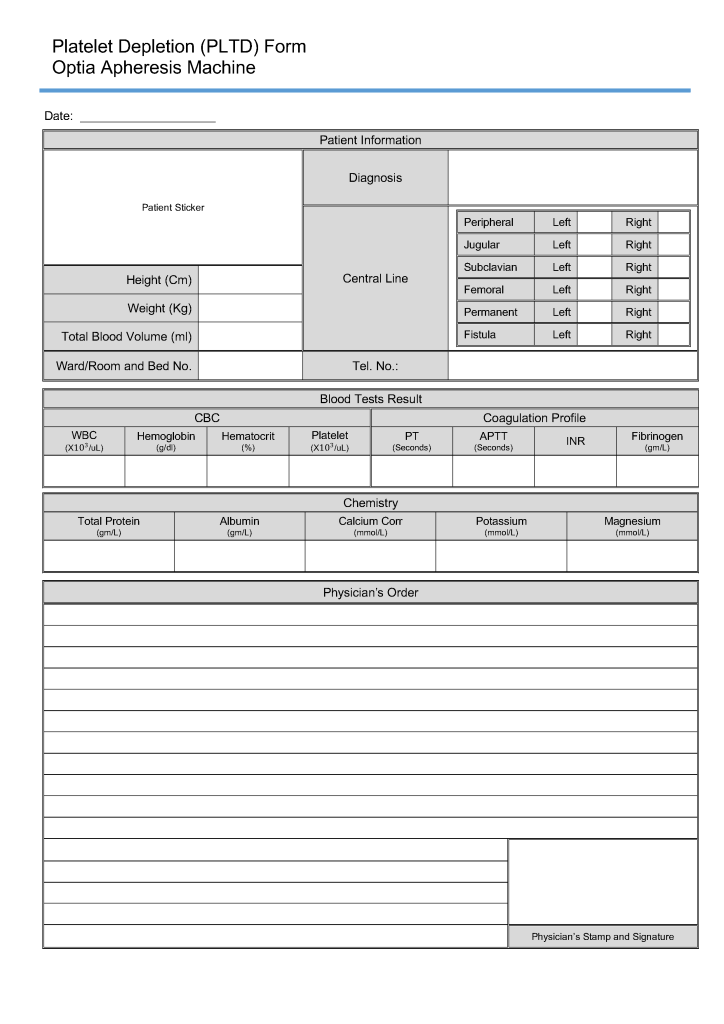
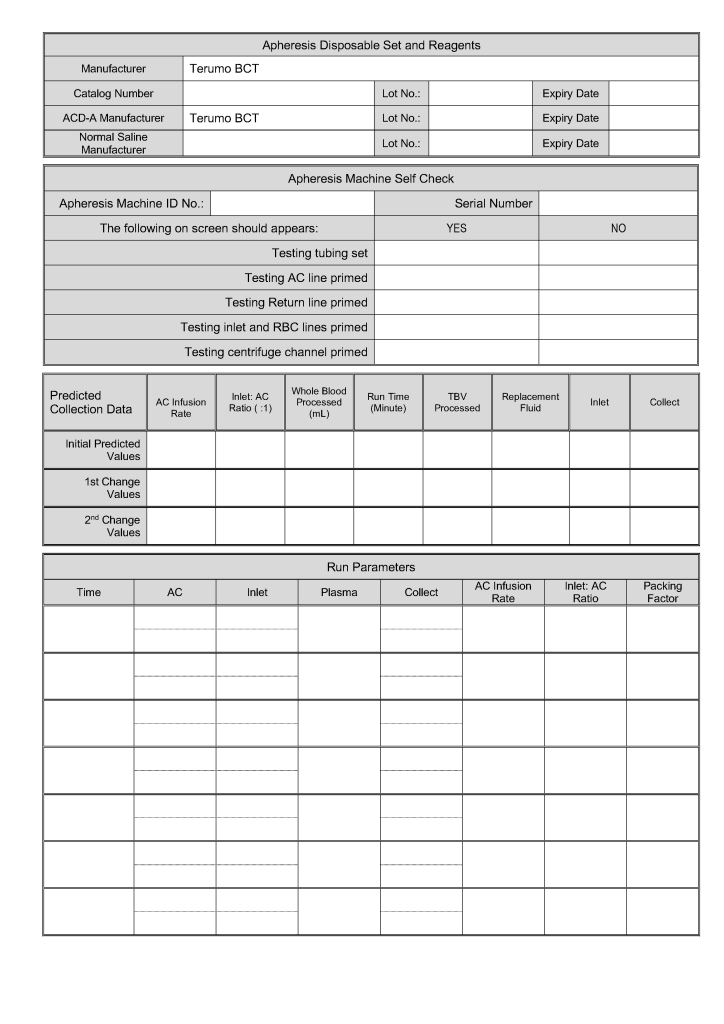
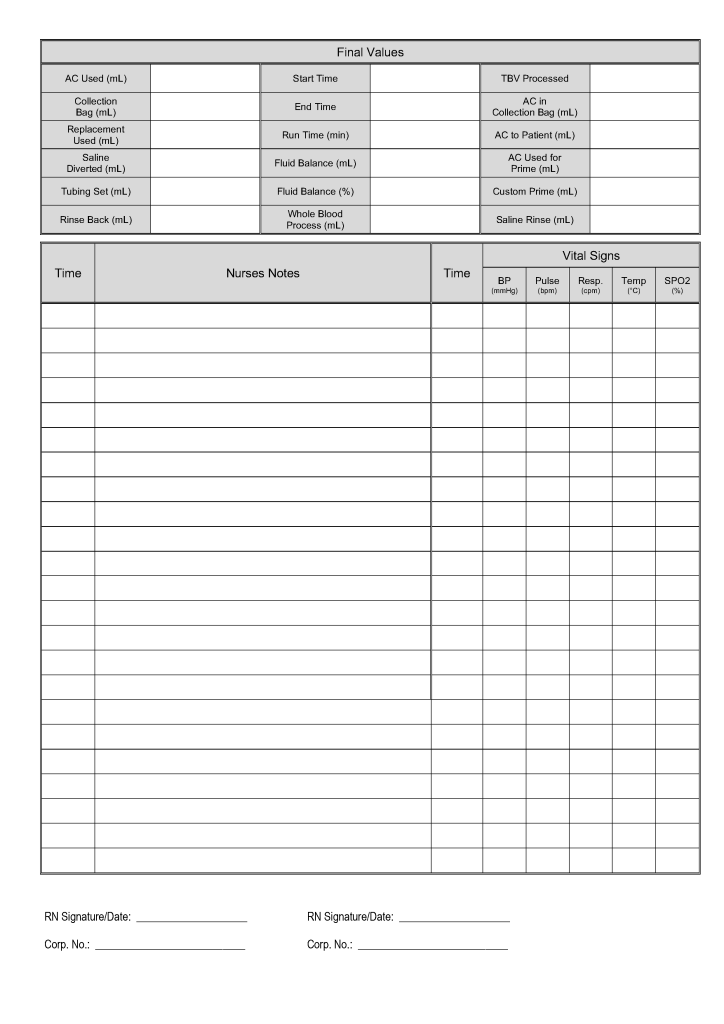
This is the sample WBC depletion form I used at several institutions in the Middle East, last updated for Terumo Optia equipment.
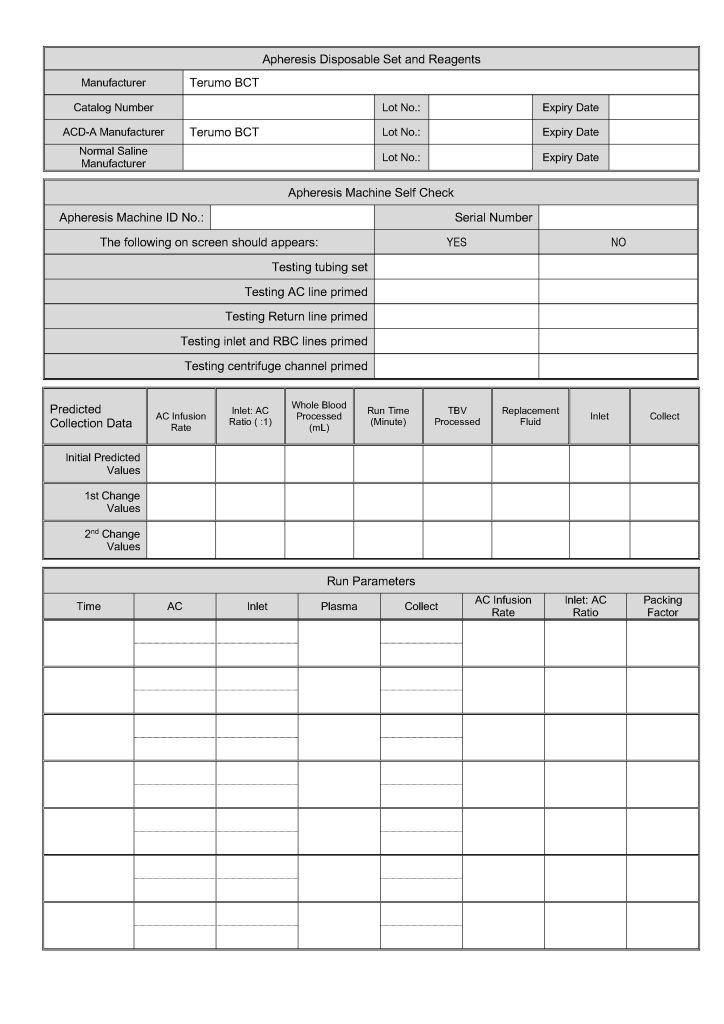
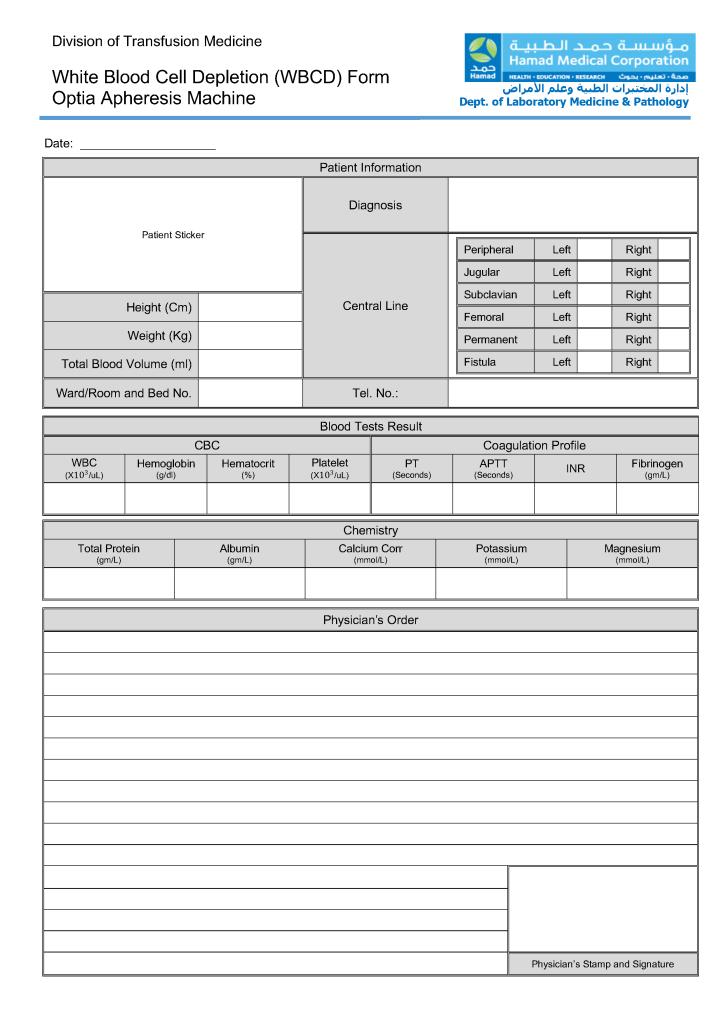

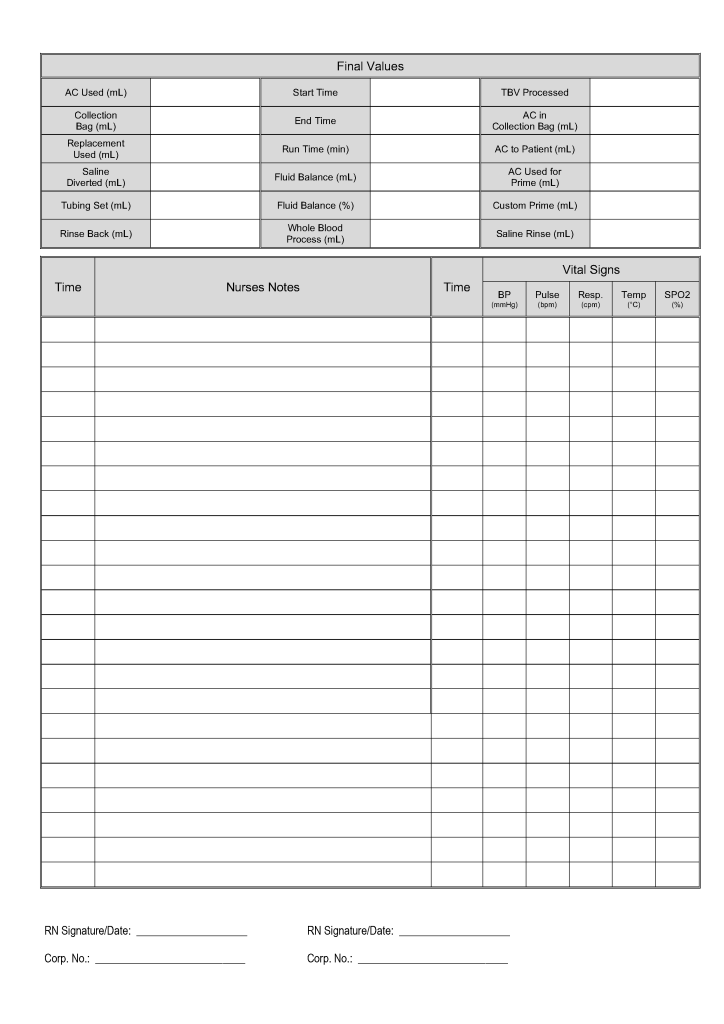

This is the sample WBC depletion form I used at several institutions in the Middle East, last updated for Terumo Optia equipment.



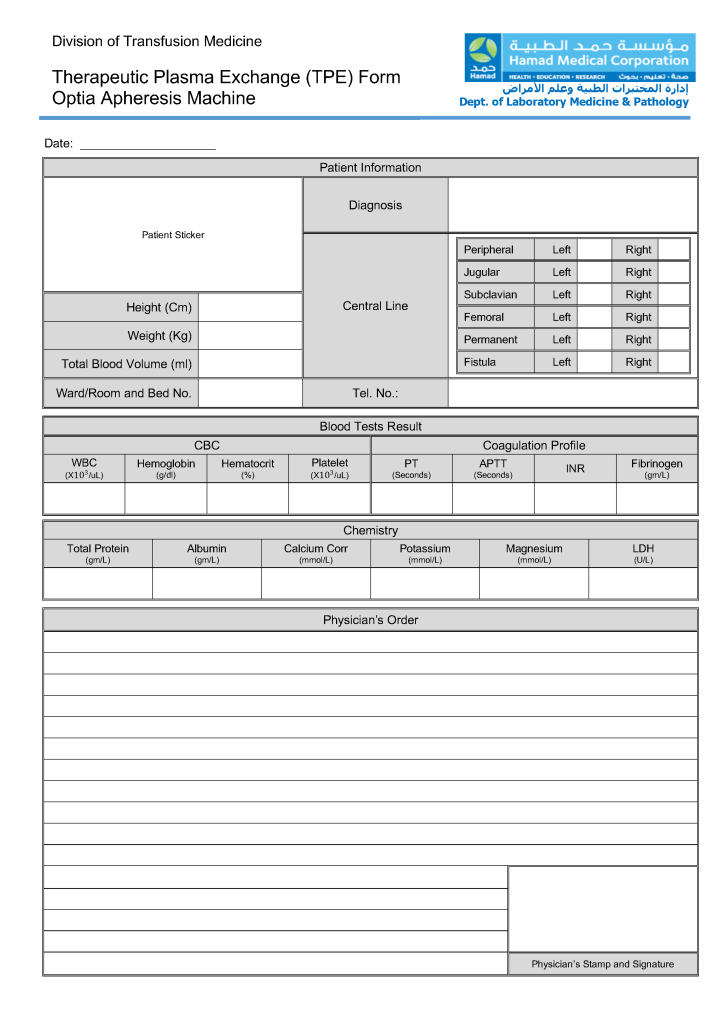
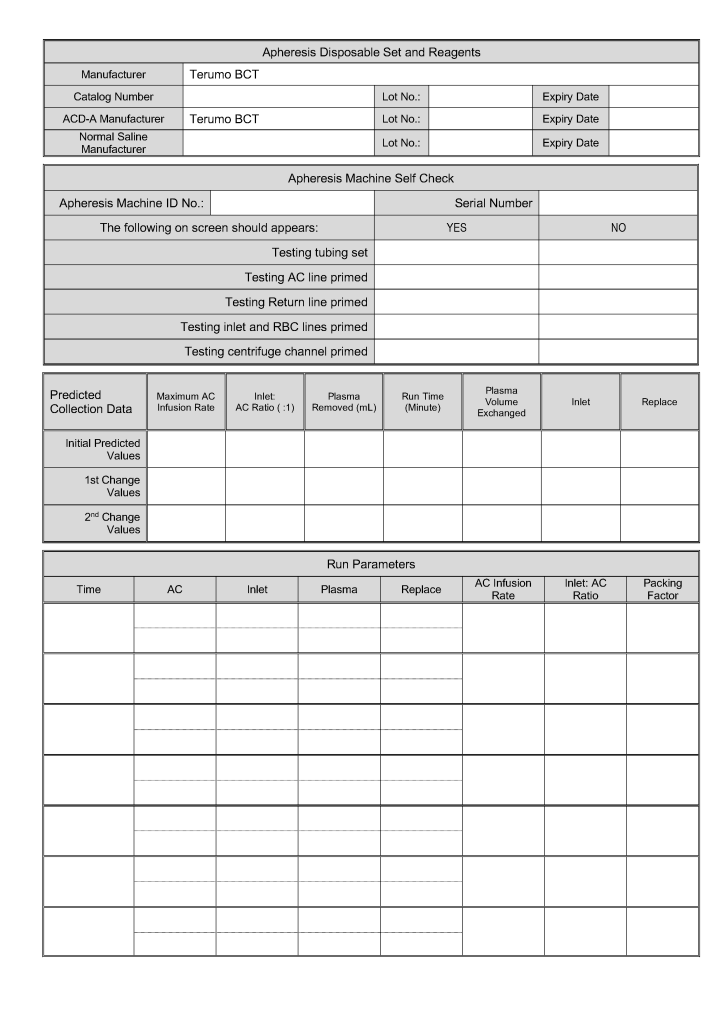
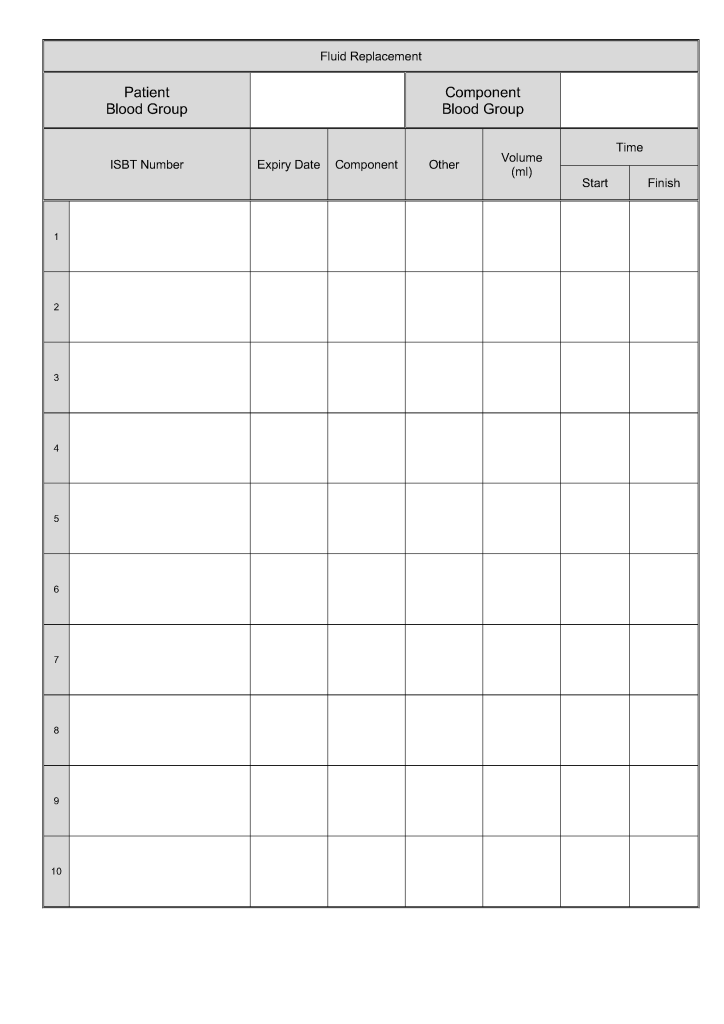
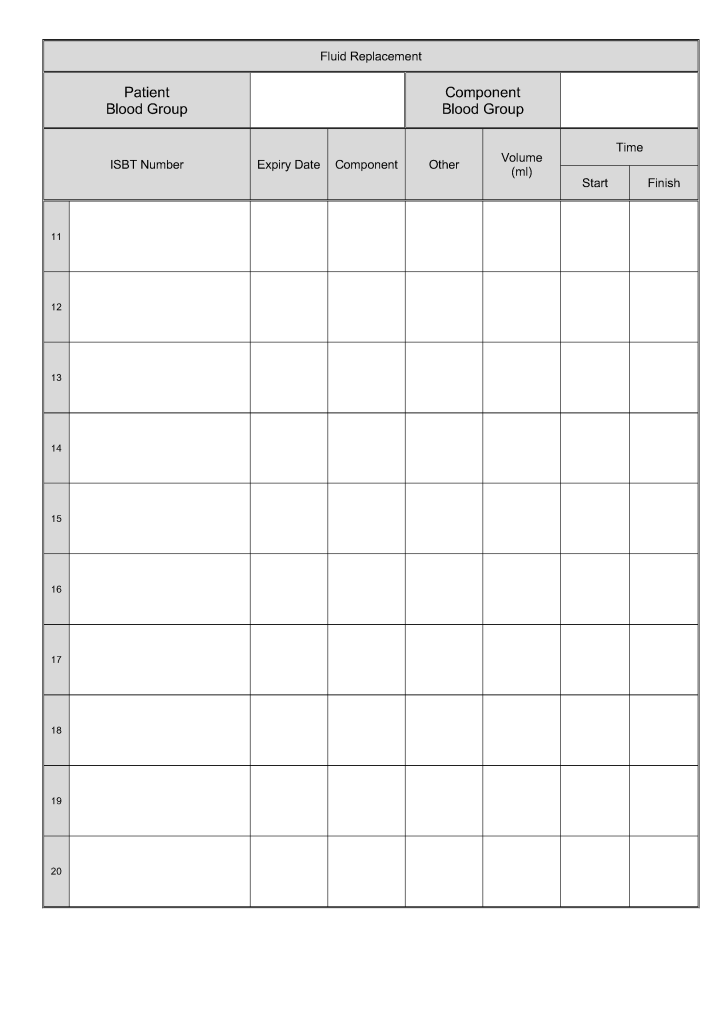
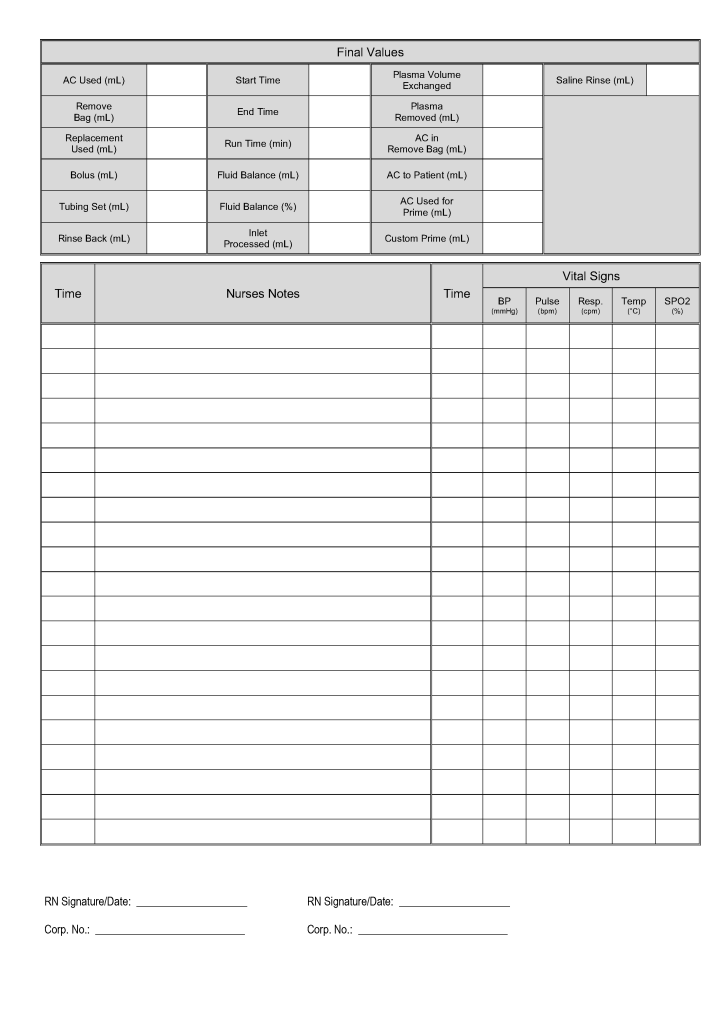
This form was developed based my experiences at several locations. It could serve as a data entry template for an electronic form.