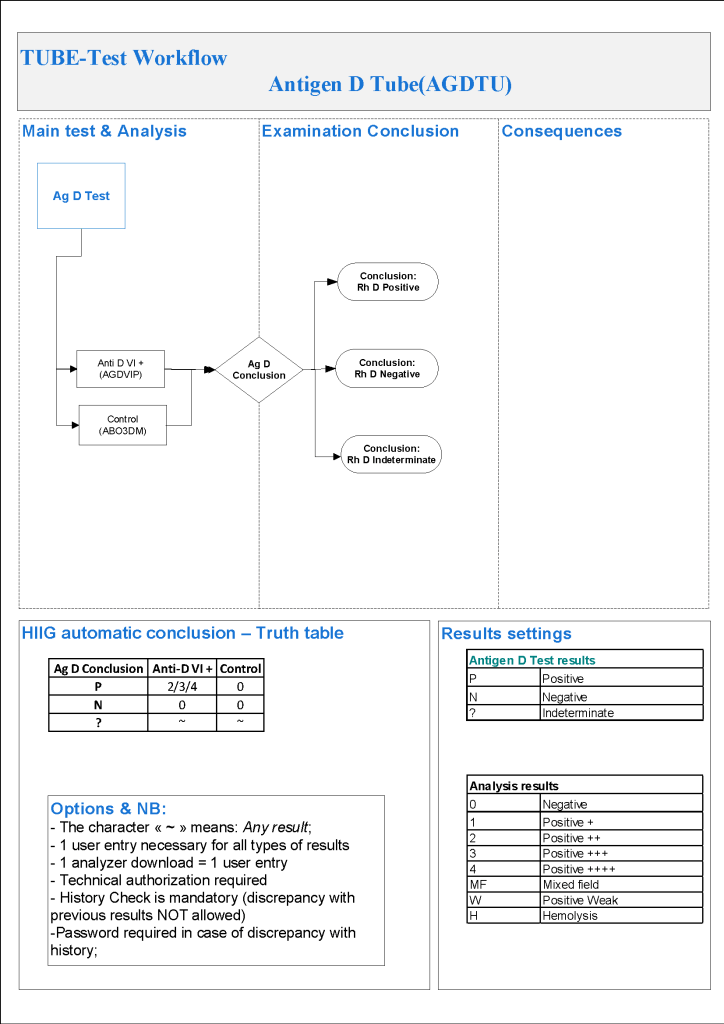
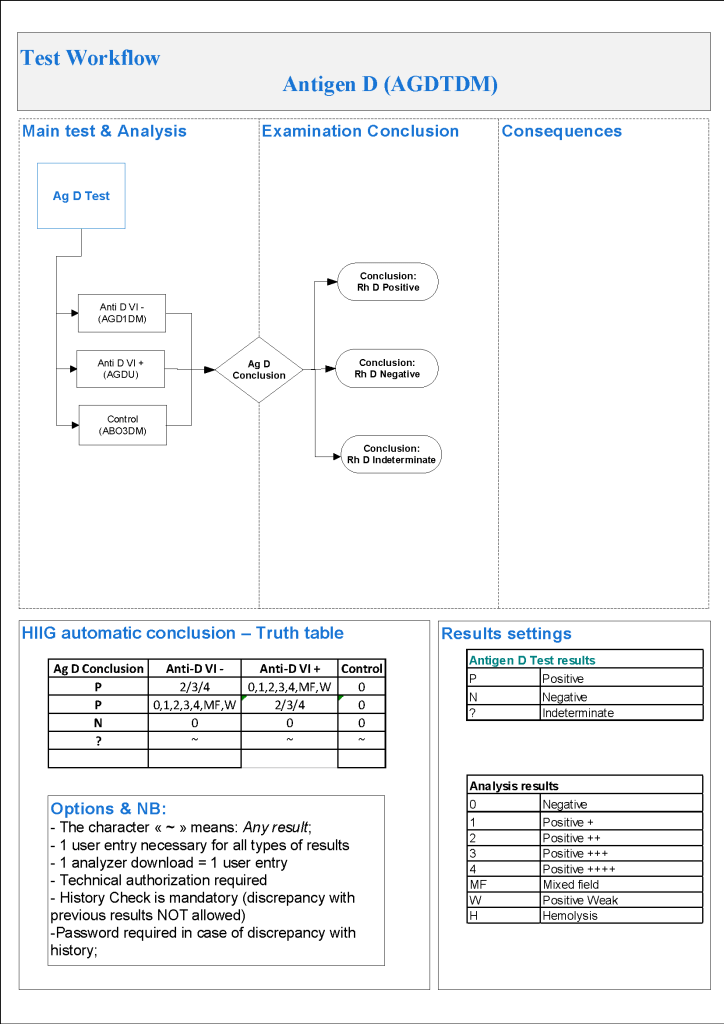
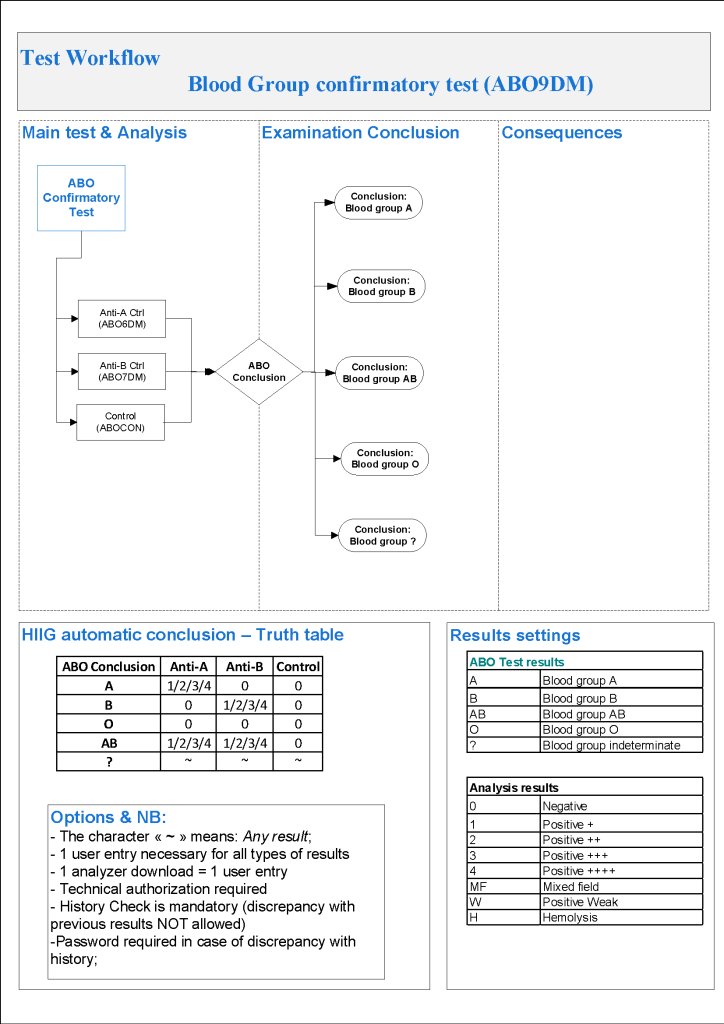
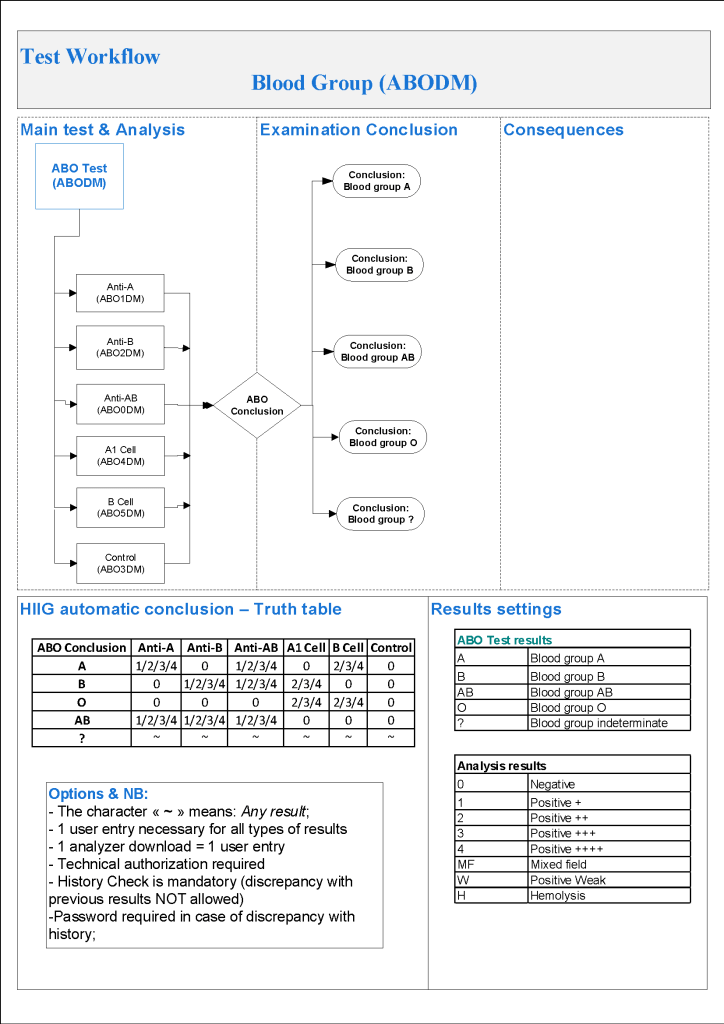
For donor antibody screening, I always had both automated and manual methods set up on the blood bank computer system Medinfo Hematos IIG. The automated method had a bidirectional interface between Medinfo and the instrument. Medinfo did not need a separate middleware. A truth table was prepared for acceptable results for automatic interpretation. Other results had to be manually interpreted by someone with the appropriate security level.
I did not use pooled cells, but instead 2, 3, or 4 cell screens at various times based on the available reagents. Personally, I prefer a 3 or 4 cell screen which is more sensitive—I want homozygous Jka and Jkb cells present. All positive cases had an antibody identification performed. According to my medical decision, I did not routinely allow any donor to be collected if he/she had a positive antibody screen. Some standards would permit the use of RBCs from such a case, but this was not my preference. In cases with rare phenotypes, I would allow production of RBCs (e.g. Bombay donor with anti-H, patient with anti-Tja (PP1Pk)) for patients with those rare types.
The manual testing option is structured similarly. Within Medinfo, it is easy to change the methodology if the system is so built. Thus, if the analyzer for antibody screening is down, the staff can select the manual methodology. Likewise, if one testing center goes off-line, the world can be completed at another site—no need to repeat testing already completed from the first site. This flexibility can apply to any test in system.
The manufacturer’s recommendations for the particular reagents in use were strictly followed. Controls were included. Most importantly, Medinfo can be configured for any set of reagent values.
Also note that Medinfo will check for the donor’s previous testing history and compare results. If there are discrepancies, this will require manual review. Normally, a donor with a positive antibody history is indefinitely deferred. The transfusion medicine physician could remove such a deferral if indicated.
Refer to the following flow diagram for a three-cell and four-cell screens.
16/10/20