Processes and Software Building—Part Three
This is an updated version of a previous post.
Using the current state to build a new work flow can be a difficult task and balancing act. If one changes it too much, it may be difficult for the staff to cope. If too little, then why bother at all? Still, we had to take the time to analyze our current system and identify areas of improvement. When building a new computer system, we didn’t want to capture our current system with its flaws in concrete. Buying a new system is costly and it would be very hard to change it again, This had to be done right.
Also, whether or not you have a pre-existing software may affect your choices. In my opinion, it is easier to learn something new than to make some changes to a system that everyone has already learned. Learning is easier than unlearning and relearning.
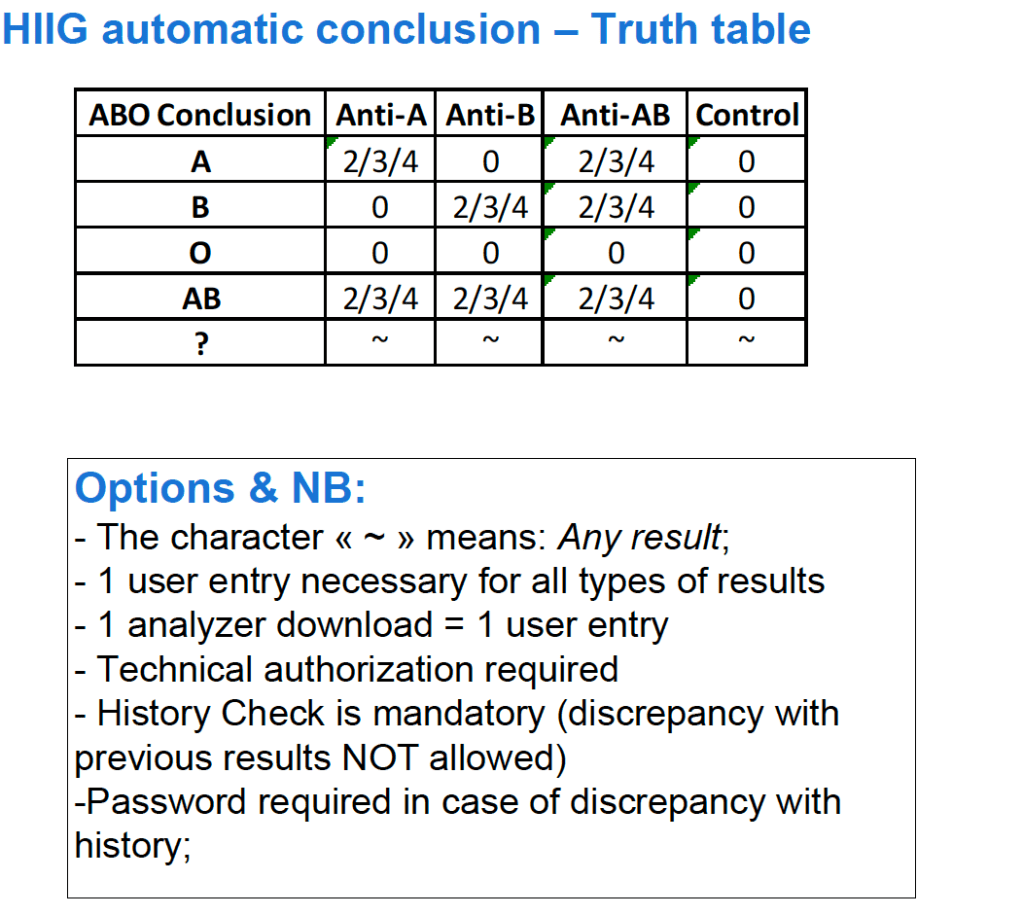
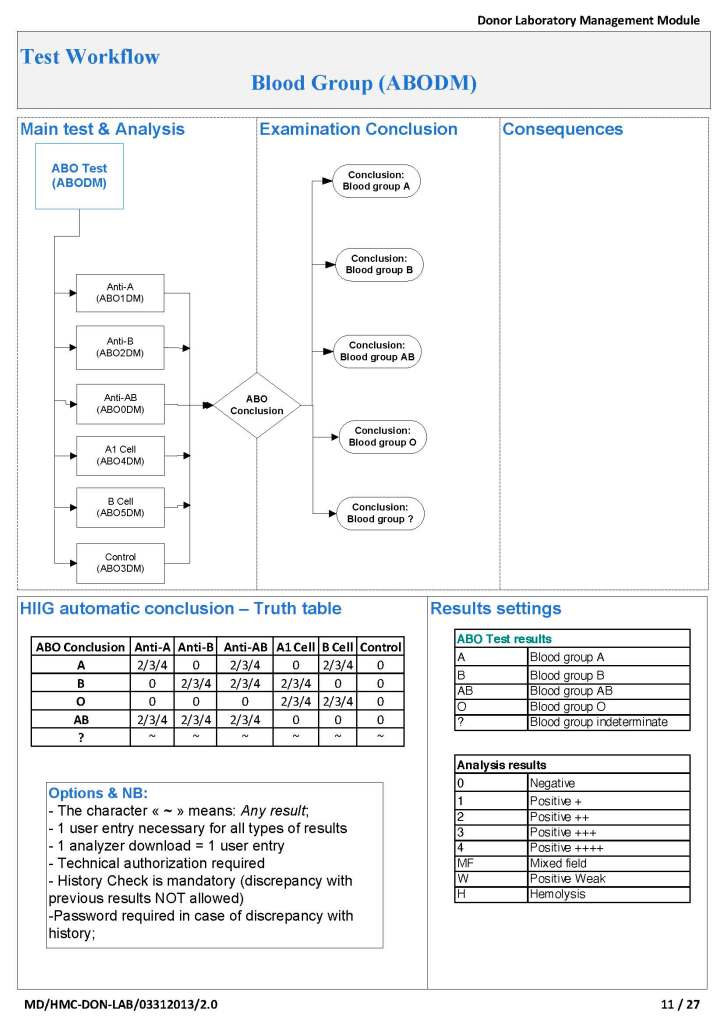
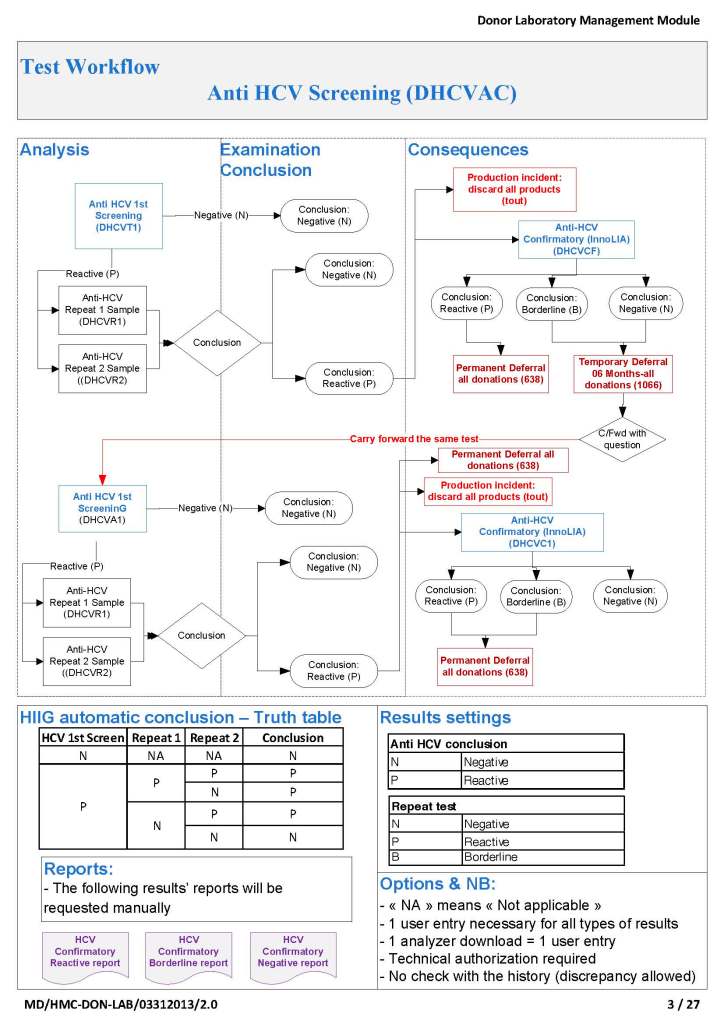
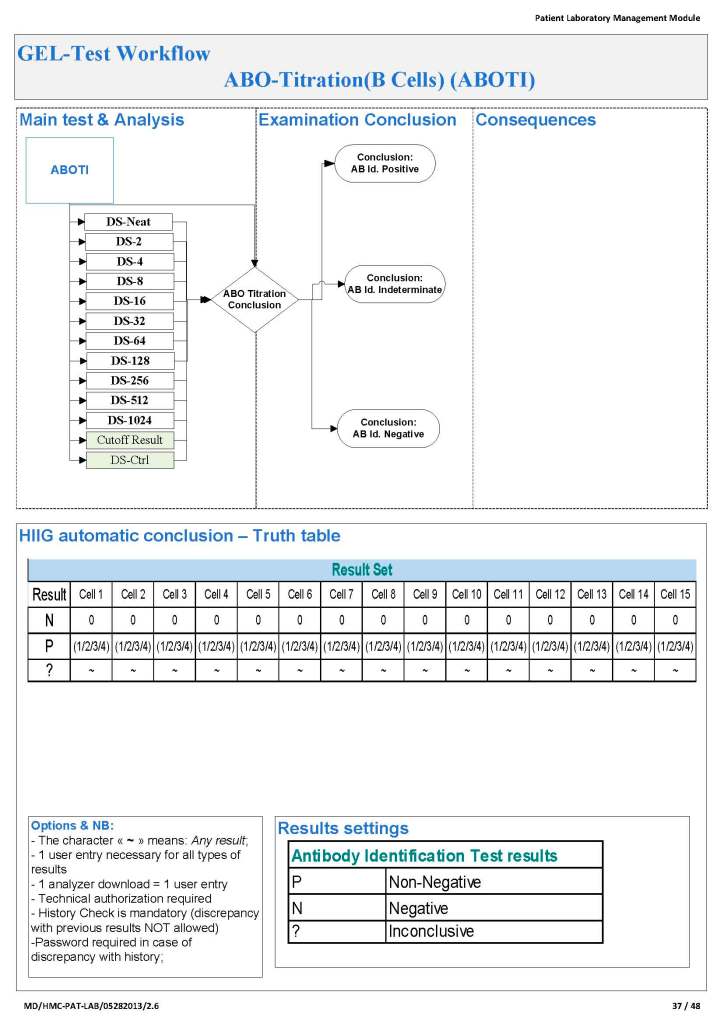
First, I studied the new system’s capabilities and took note of the features I would like to adopt to improve the current processes. I did this especially at the critical control points. I also studied our incident reports: where had there been nonconformances? How could I change things for the better, i.e. with increased safety and compliance to international standards?
I did not want to throw out a successful manual system, just to optimize it. I tried to pick out those manual processes that worked and build those into the new workflows. What I wanted was a system recognizable and familiar to the staff but with enhancements with the least amount of change to reach our goals.
Although the vendor did some initial testing, this was insufficient to accept the system. I didn’t want the vendor to just show me some scenarios that they concocted. I was always suspicious why the vendor chose these examples and not others. Could it be that the other processes did not work as desired? I always insisted that I give the vendor representative scenarios and have them show me how the system reacted.
It is daunting task to know what settings to make. At one of my previous institutions, the administration recognized that they needed additional expertise from someone experienced in the new system. They hired an outside firm in addition to the software vendor. Still, even this was not sufficient to make the proper settings and testing. We had to rely on ourselves!
Ultimately, the Laboratory had to thoroughly test the system, The only way to do this was to use our own resources. Only we could test its actual functionality to the proper degree to ensure safety. Still, where could we get the resources to do this? Outside consultants were very expensive, especially if they have to live on-site for extended periods. The only answer was to make use of our internal resources, i.e. our staff.