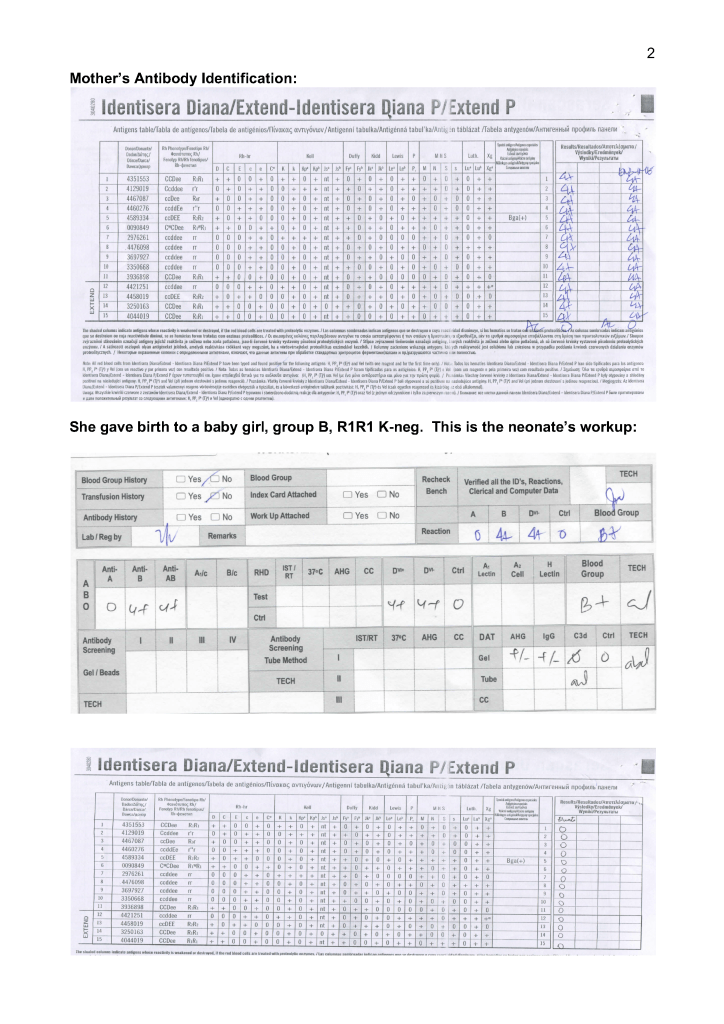
Includes compatibility testing (AHG, electronic, immediate-spin), antigen typing, antibody screening and identification, direct antiglobulin testing, elution, transfusion reaction and drug reaction workups, component typing tests upon receipt in hospital blood bank, release and return of components